Health Insurance Platform
Designing a three-sided system
for patients, hospitals, and insurers — YHealth
INITIAL STATE
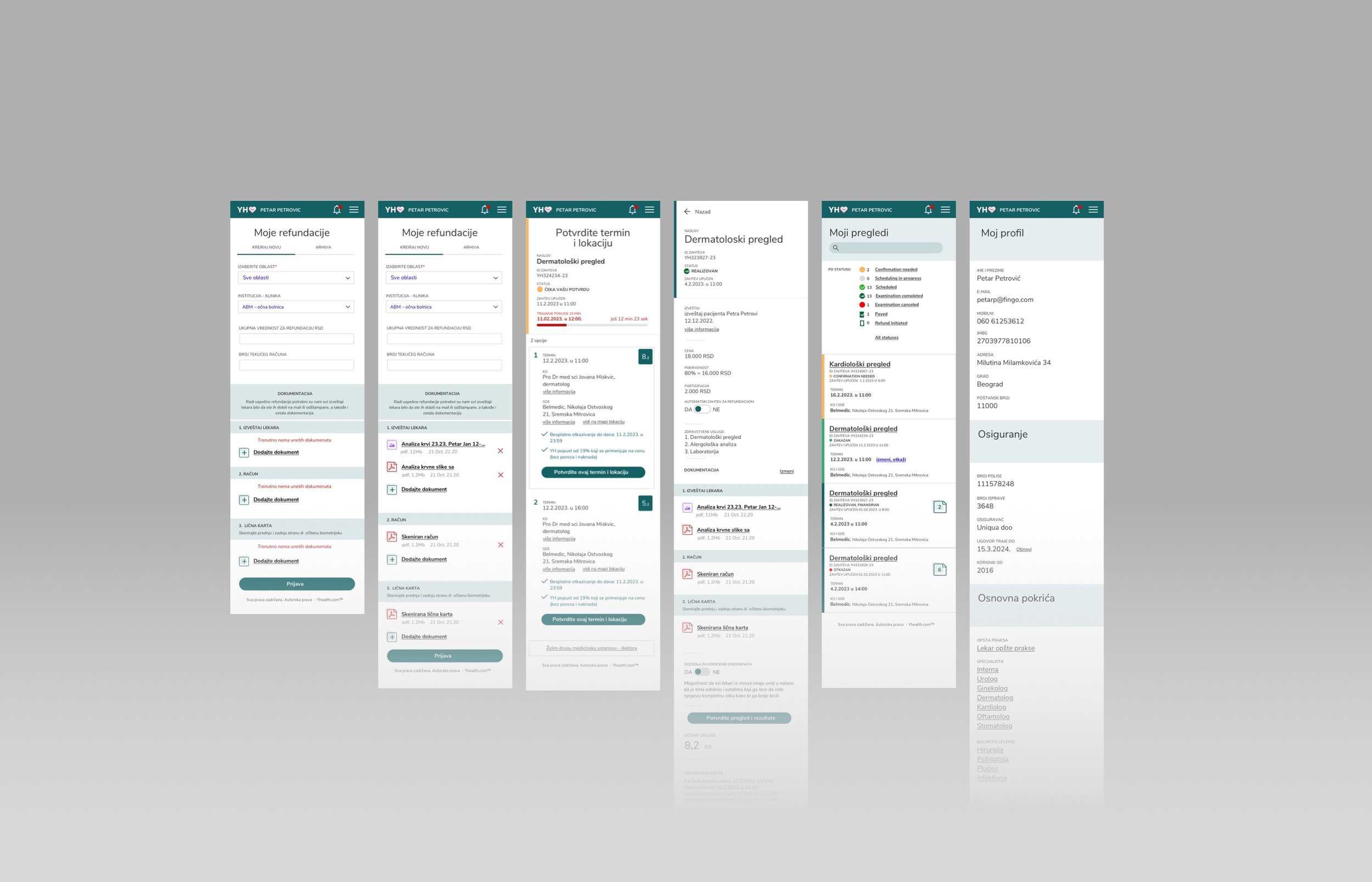
Health insurance is one of the most friction-heavy experiences in a person's life — claims that disappear into bureaucratic processes, appointments that require multiple calls to coordinate, records scattered across providers and insurers with no unified view. YHealth was built to address exactly this: a platform connecting patients, hospitals, and insurance companies in a single system.
The challenge wasn't just complexity — it was sensitivity. Every piece of data in the system is either medical, financial, or both. Every workflow touches regulatory compliance. And every user group — patients managing their own care, hospital staff processing claims, insurance administrators approving coverage — has fundamentally different needs, permissions, and mental models.
The Ask
Design a unified platform across three distinct interfaces: a consumer-facing mobile app for patients, a desktop system for hospital and insurance company staff, and an administrative layer for managing the approval chain between them. The design needed to maintain strict data separation between user roles while creating a coherent experience across all three surfaces.
SOLUTION
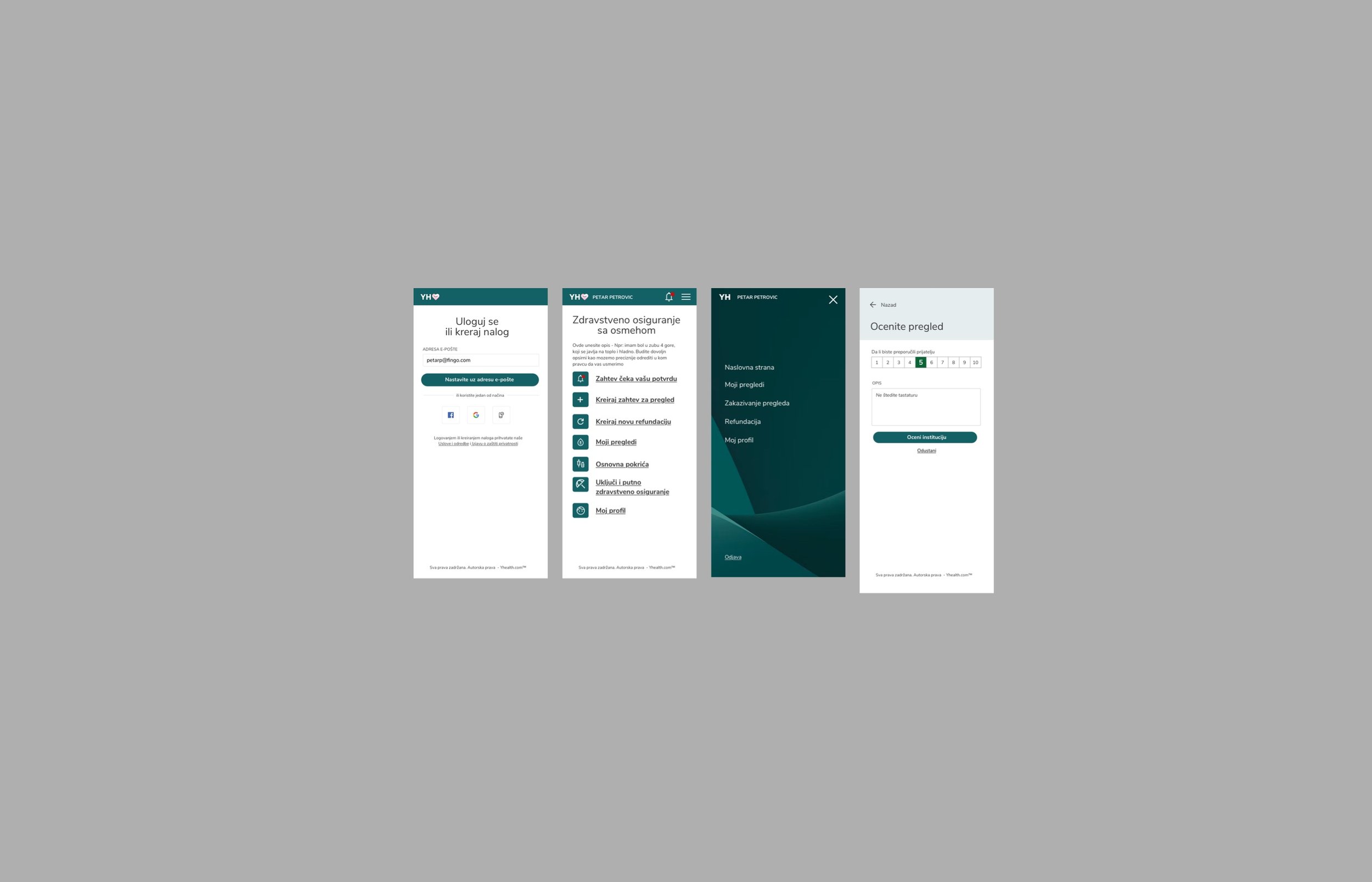
The core architectural decision was to treat each user group as a completely separate product sharing a common data layer — not a single interface with role-based visibility toggles. Patients needed simplicity and reassurance. Hospital and insurance staff needed density, efficiency, and auditability. Mixing those needs in a single interface would have served none of them well.
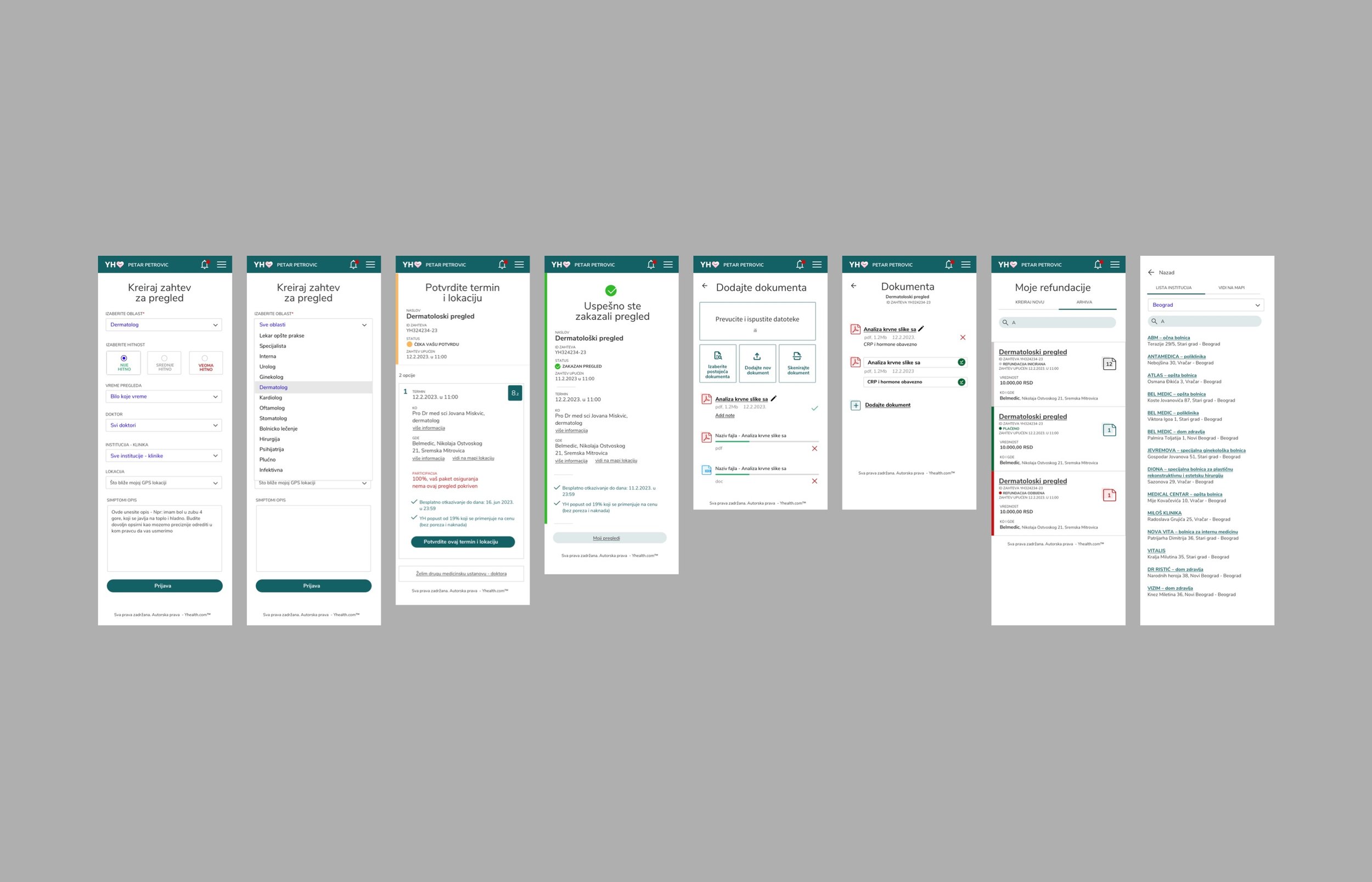
The patient app was designed around reducing anxiety, not just completing tasks. Insurance information is inherently stressful — claims, coverage limits, approvals. The interface surfaced status clearly and proactively: where is my claim, what is covered, what happens next. Real-time updates eliminated the need to call to find out. Health tracking and appointment scheduling were integrated to make the app a daily utility, not just a claims tool opened in moments of stress.
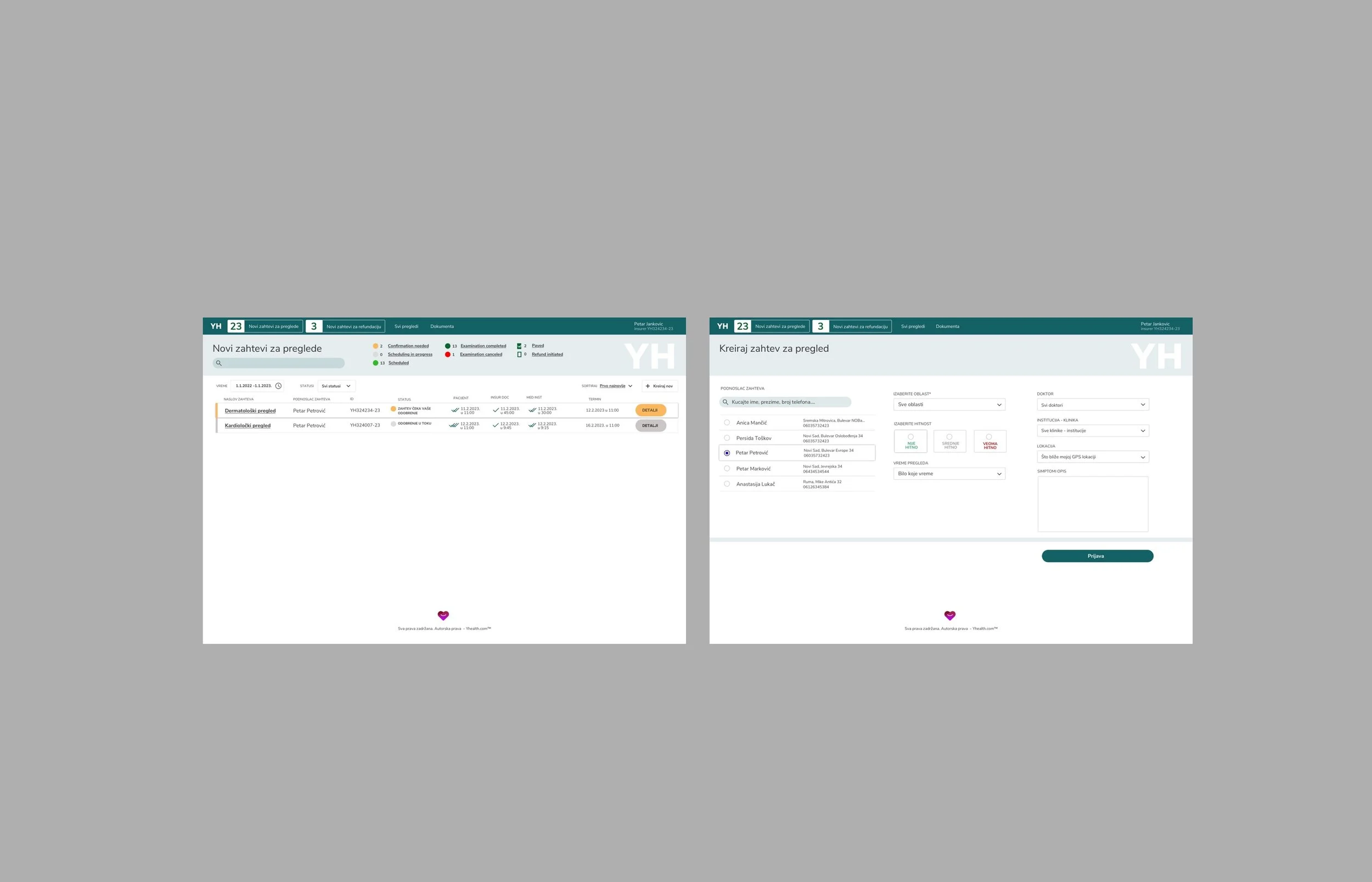
The desktop system for hospitals and insurers was built for workflow efficiency under regulatory constraint. Claims processing required a clear audit trail — every approval, rejection, and modification logged with timestamp and user. The dashboard surfaced workload by priority rather than chronology, ensuring time-sensitive approvals didn't get buried in volume. Role-based permissions were designed to be granular enough for compliance without creating friction for legitimate daily tasks.
The approval workflow connecting all three surfaces was the most complex design challenge. A patient submits a claim, a hospital validates treatment records, an insurer reviews and approves coverage — each step with its own stakeholder, timeline, and data requirements. The interface made the chain of custody visible to all parties at their appropriate permission level, eliminating the black box that makes insurance processes so frustrating.


IMPACT
YHealth brought transparency to a process that typically operates in the dark. Patients gained visibility into their claims without needing to call. Hospital staff processed approvals faster through a prioritized workflow. Insurance administrators maintained compliance through built-in audit trails. The platform demonstrated that highly regulated, multi-stakeholder systems can be designed for clarity — not despite their complexity, but by taking it seriously.
